|
The assessment of patients in services starts with their oxygen saturation as measured by a Pulse Oximeter, SpO 2, followed by consideration of other signs and symptoms. Those aged over 65 and/or with multiple comorbidities defining them as extremely vulnerable are being targeted by the pathway due to a higher risk of deterioration (NHSE, 2020a). 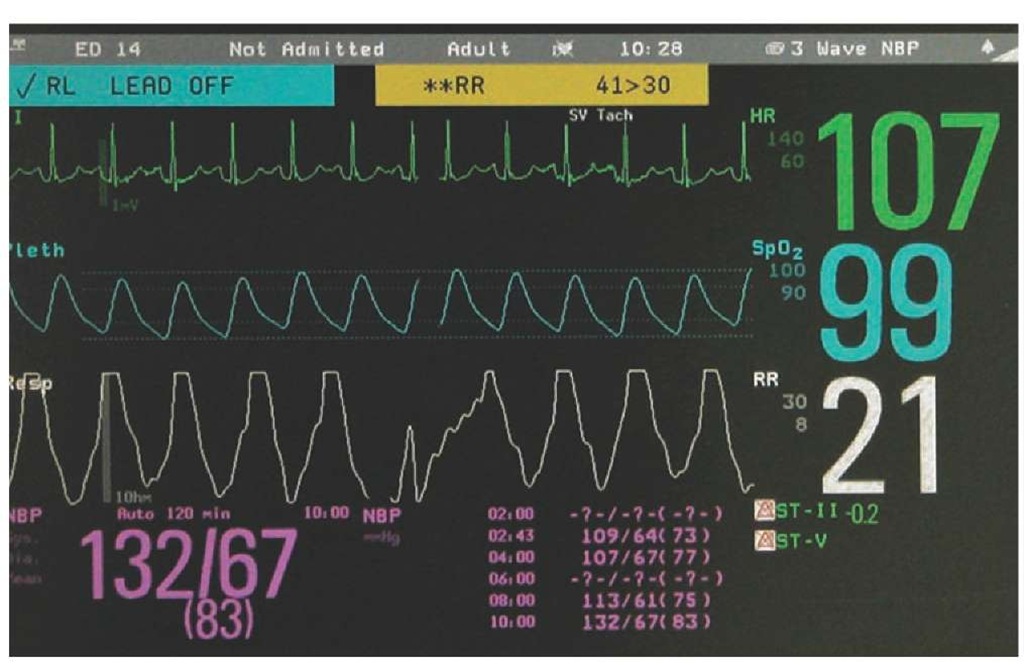
Patients are given instructions on interpreting their results so they can act independently if they need to, such as seeking urgent care. The App either gives an automated response/recommendation, or data are monitored by a clinician who can contact the patient if necessary, though usually only during normal working hours. Patients referred to services are usually directed to use an App or a paper diary to record their observations. 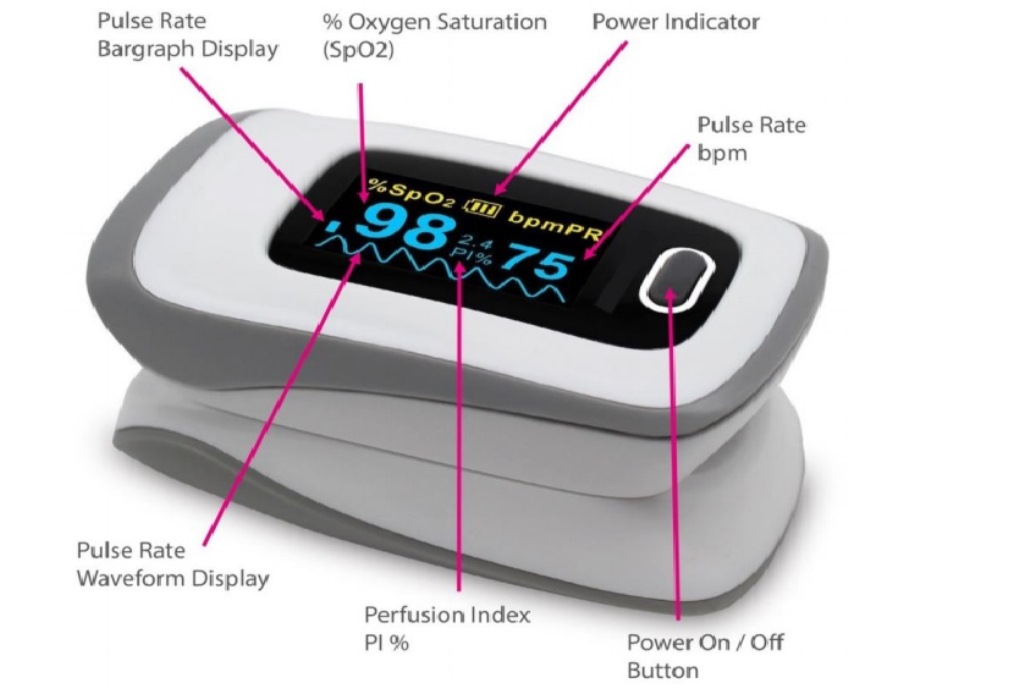 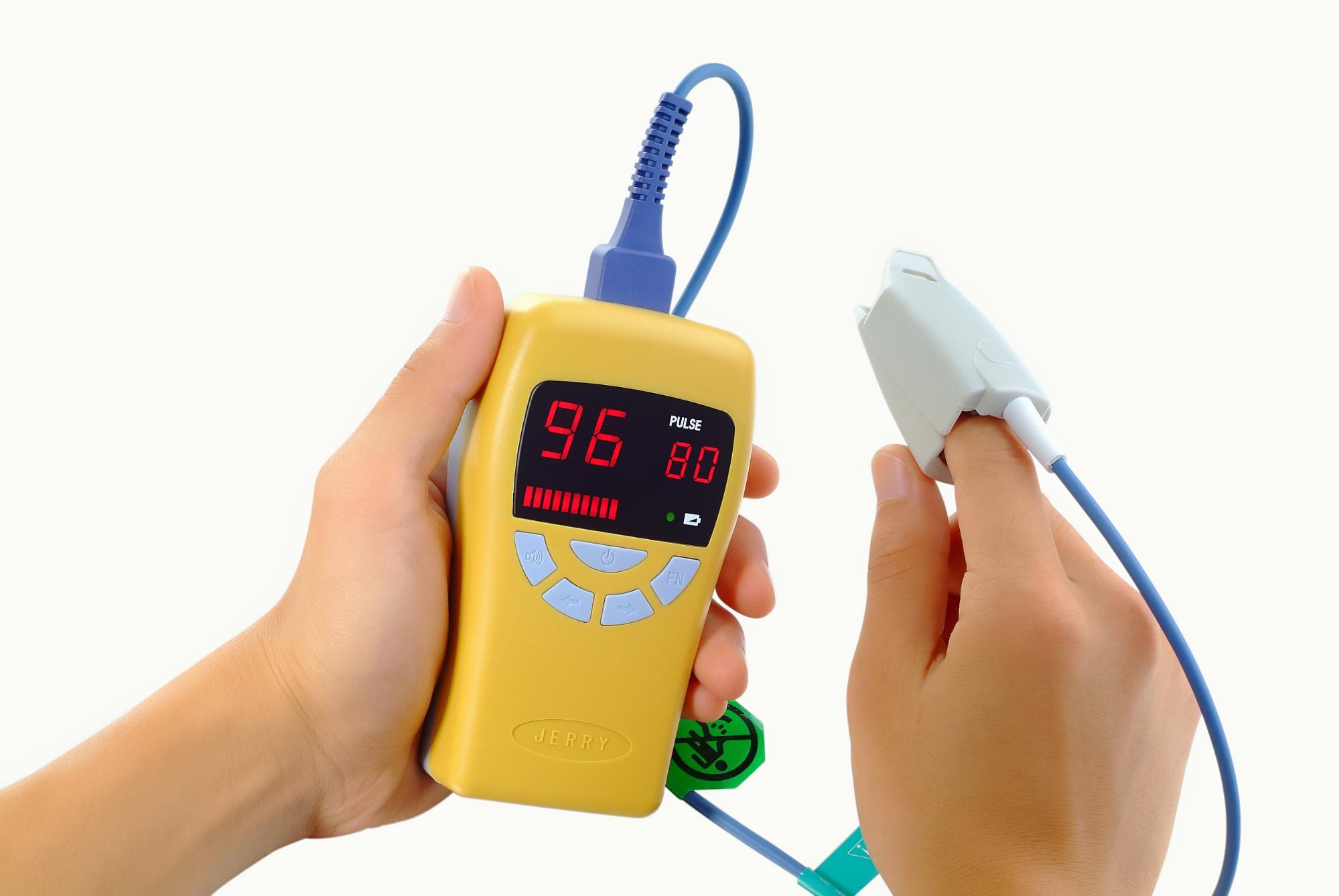
With the usefulness of patient performed home-based pulse oximetry in both preventing unnecessary emergency department attendance (Torjesen, 2020) and in early identification of silent hypoxia, however, NHS England has recommended national commissioning of services (NHSE, 2020a) where patients with mild COVID-19 symptoms but at higher risk of deterioration can be given with a Pulse Oximeter for 14 days in order to self-monitor their oxygen saturation (SpO 2) 2–3 times a day. There are a number of advantages in managing less-serious cases of COVID-19 in the community, though this limits, the use of medical devices such as thermometers, stethoscopes and pulse oximeters during the assessment.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
